What is leprosy?
Leprosy still causes disability and social exclusion. It affects millions of lives.
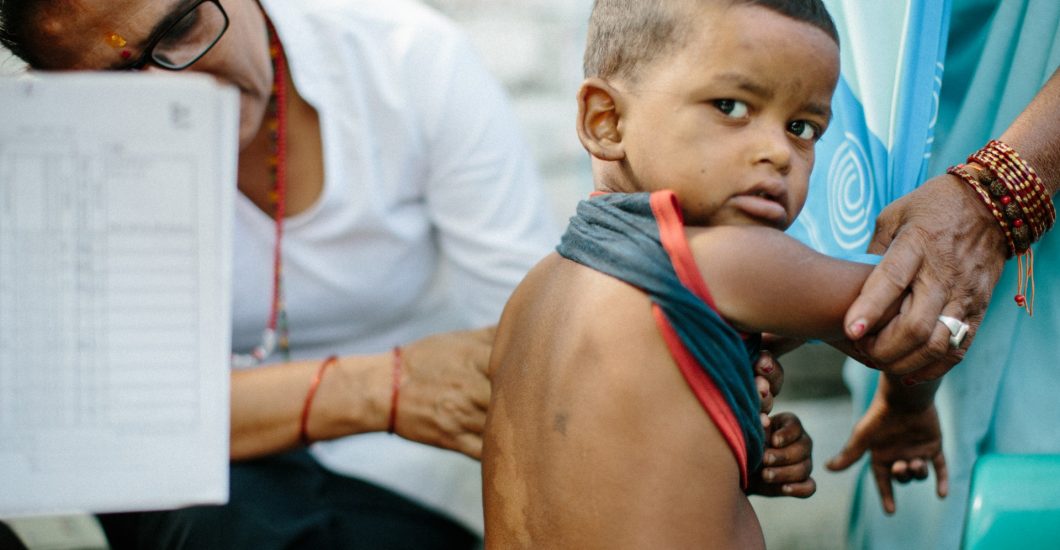
Key facts
- Leprosy (also known as Hansen’s disease) is an infectious disease caused by a bacillus, Mycobacterium leprae.
- M. leprae multiplies slowly, the period between infection and seeing symptoms (incubation period) is long and can vary between 1 year and 20 years (5 years on average)
- During the incubation period, an infected person does not yet have any visible signs or symptoms but may already infect others.The disease mainly affects the skin, the peripheral nerves, and the eyes.
- The first symptom of leprosy is often the occurrence of skin patches without sensation (anaesthetic), that are lighter or darker than the person’s overall skin tone.
- Leprosy is curable with multidrug therapy (MDT). MDT is available to leprosy patients free of cost.
- Leprosy is not a highly contagious disease. It can spread from person-to-person by prolonged close contact (as may occur in a household) with a person who is not taking or who has not completed treatment , via droplets from the nose and mouth.
- Without timely diagnosis and treatment, leprosy can cause progressive and permanent damage to the peripheral nervous system, the soft tissue of the nose and throat, and vision.
Leprosy potentially has severe long-term consequences if not detected and treated in time. That’s why NLR continues to fight leprosy until No Leprosy Remains.
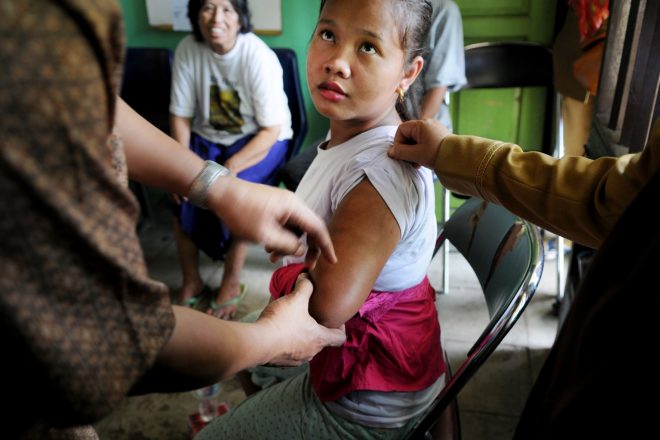
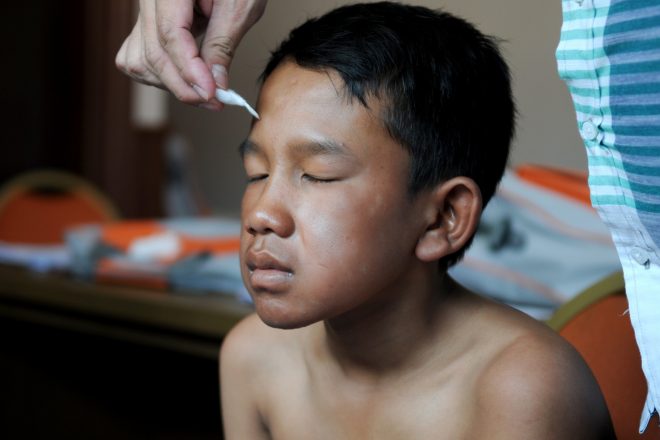
Physical and social impact
If left untreated, leprosy can cause progressive and permanent damage to the peripheral nervous system, the soft tissue of the nose and throat, and vision. Due to a loss of sensation in the extremities, persons affected by leprosy easily injure themselves . These, often painless, injuries may become infected, which may eventually result in tissue loss in affected areas such as in the fingers and toes. Timely diagnosis and treatment are crucial to prevent impairments and disabilities. It is estimated that 2-3 million people are living with leprosy-related disabilities globally. These people are cured, but have lasting impairments.
The visible impairments associated with leprosy are an important contributor to stigma. Persons affected by leprosy who have physical impairments can for example be perceived as dangerous, which makes people want to keep their distance. Fear of getting infected, poor knowledge of leprosy and religious and cultural beliefs all contribute to stigma. Many persons affected by leprosy are also affected by stigmatization. Stigma can affect and disrupt many areas of the affected person’s life, but may also impact the lives of their family members, and influence diseases management. In general, among community members there is low awareness and lack of knowledge about the cause, mode of transmission, early symptoms and contagiousness of leprosy. This also contributes to stigma, negative attitudes and discrimination towards persons affected by leprosy.
Leprosy creates vicious cycle of poverty
Extremely poor people are at particularly high risk of developing leprosy, because the socioeconomic and physical conditions in which they live create environments that facilitate the transmission of leprosy. Research has shown that they are systematically excluded and derive very little benefit from development or health care interventions in general. Women experience particular disadvantages. The negative psychosocial consequences of leprosy, and the risk of developing disabilities, can put poor patients in a vicious cycle of poverty, stigma, unemployment, social exclusion, and mental distress.



Millions of people are still at risk
In 2019, the number of new leprosy patients reported globally was 202,185. The geographical distribution of leprosy is uneven, 80% of the world’s leprosy patients live in three countries: India (57%), Brazil (14%) and Indonesia (9%). Of the new patients detected globally in 2019, 7% were children and 5% had grade two disabilities at diagnosis. These are indicators of ongoing transmission and of late diagnosis of leprosy. In addition, these percentages indirectly provide information about community and health staff awareness about leprosy and the quality of leprosy services. The problem with these official figures of annual new cases is that they only reflect patients that sought medical assistance and were recorded in the national data for each country. They do not include those people that either have not yet manifested symptoms or were misdiagnosed. These people can infect others for years before leprosy is diagnosed Furthermore, the official numbers do not include the contacts of leprosy patients who run the risk of contracting the disease. Research done by Erasmus MC and NLR, shows that even by modest calculations, millions of people are still at risk.



Towards zero leprosy
A breakthrough and potential game-changer in the fight against leprosy is the introduction of prevention of leprosy, by prescribing a single dose of rifampicin (an antibiotic that is also part of MDT for leprosy patients) as “post-exposure prophylaxis” also known as SDR-PEP to contacts of newly-diagnosed leprosy patients. The treatment reduces the risk of contacts developing leprosy by nearly 60%. In 2018 the WHO included SDR-PEP in the Guidelines for the Diagnosis, Treatment and Prevention of Leprosy. NLR strives to promote the implementation of SDR-PEP as widely as possible, believing that it will be a definitive step towards zero leprosy. Moreover, In an attempt to find a more effective regimen for the prevention of leprosy, NLR launched the “Stop the Transmission of Leprosy! Project” in 2017.

until No Leprosy Remains
NLR is a global forerunner towards a leprosy free world. We promote and support prevention and treatment of leprosy, prevention of disabilities, social inclusion and stigma reduction. We focus on Three Zeros.